
Gender Identity
What does it mean to have your sex assigned at birth?
When a baby is born the socially expected interaction goes something like “Congratulations Mrs Smith, you have a healthy baby boy (or girl)”. Leaving aside the relationship status assumption, the sex assigned at birth relies on the visible genitalia of the baby. This is the same method used by ultrasound scans if the parents want to know before the child is born. This technique would be right most of the time, but it does not cater for the approximately two people in every thousand who do not fit the sex binary. There are subtle variations in chromosomes, hormone function, brain structure and experiences while in the womb that can produce something in between. The conclusion is that biological sex is not binary, because it cannot be grouped into two separate, non-overlapping groups. It is more accurately described as bimodal, which means that there is a continuum from male to female with two statistical peaks representing what we would classically call male and female.
What about gender?
Once a baby has had their sex assigned at birth they will probably be raised as if they were that sex. There is an unspoken assumption that they will be happy to adopt the gender associated with their assigned sex. Typically if they are assigned to be male they will be acculturated to become masculine. If they are assigned to be female they will be acculturated to become feminine. Along with the social conditioning and expectations (like pink or blue clothing) it seems reasonable that there are genetically derived attitudinal dispositions associated with being male or female. Gender Identity represents the suite of proclivities that inform an individual as to how they fit into the current social model of continuum from masculine to feminine. This can be mixed or binary as well as fluid. Gender Expression is the extent to which an individual lives out their gender identity. It seems likely that social pressure is the main factor that limits free gender expression.
So what is ‘cis’ and ‘trans’?
If, as is most commonly the case, a person’s gender identity aligns with the sex they were assigned at birth they are called cisgendered. There are those for whom this is not the case, and they must endure the extreme distress of inhabiting a body that does not match their gender identity. The term for this is transgender and it applies whether or not the individual has, or is seeking to transition to the body type associated with the other sex. The current term to frame the distress suffered by trans people is gender dysphoria.
This has nothing to do with sexual orientation
Who we are sexually attracted to (if we experience sexual attraction) has nothing to do with our gender identity except to the extent that society likes to apply labels such as straight, lesbian, gay or bisexual in order to classify the various forms of sexual connection. Modern understanding is moving towards an acceptance of a continuum and fluidity across all the aspects of human diversity. It’s worth noting that this can introduce yet another subtle pressure on those who identify as transgender, as they may feel attuned to the binary model in order to frame the start and end point of their transition.
What can a trans person do?
Depending how evolved the culture was in which a trans person grew up, it may be some time before they come to an understanding of their distress. For similar reasons it may be some time before they feel safe enough to consider their options. While there may be many ways to find a liveable accommodation with their situation, for some the only satisfactory resolution is to change their body to better match their identity. This is know as transition, and involves medical interventions, both pharmacological and surgical, which carry risks. It’s not just medical risks that must be faced, but complex psychological, legal and social issues to navigate. In the UK there is a pathway for transition available on the NHS but it can be underesourced and bureaucratic. Many of the cosmetic procedures that will help a trans person ‘pass’ for their preferred gender identity are expensive. Untangling previous legal structures (such as marriage) and obtaining a gender recognition certificate can be complex and time consuming.
Psychological support
Trans people are regular people who face all the regular problems of life so it can’t be assumed that if they seek therapy it’s because of their trans status. Psychological support for a trans person (or their family) through their journey of transition can benefit from onward referral to therapists who specialise in this area.
Transition
If a trans person has decided they want to transition to a body style that represents a match to their gender identity they have a long and complex journey to undertake. The journey may expose them to discrimination and prejudice. The current NHS pathway initially involves a GP referral to a Gender Identity Clinic for assessments of the client’s gender dysphoria and the idea of a trial to live in the preferred gender. There would be an individual care plan which attempts to cater for all the implications of a shift in gender expression, including the effect on family and employment circumstances. The Gender Identity Clinic would assist with appropriate psychotherapy and speech therapy. The provision of hormone therapy is only released after two independent clinicians agree. Hormone therapy helps the body shift gender characteristics but does not change physical features. That requires surgery with all the inherent risks. There are specialist services to cater for the particular needs of the trans community. Check out these specialist resources: www.cliniq.org.uk and www.brightonsexualhealth.com/service/clinic-t
Which way?
The transition from male to female (MtF) involves different procedures and challenges from the transition from female to male (FtM). In both cases transitioning involves taking cross sex hormones (oestrogen and antiandrogen for MtF and testosterone for FtM).
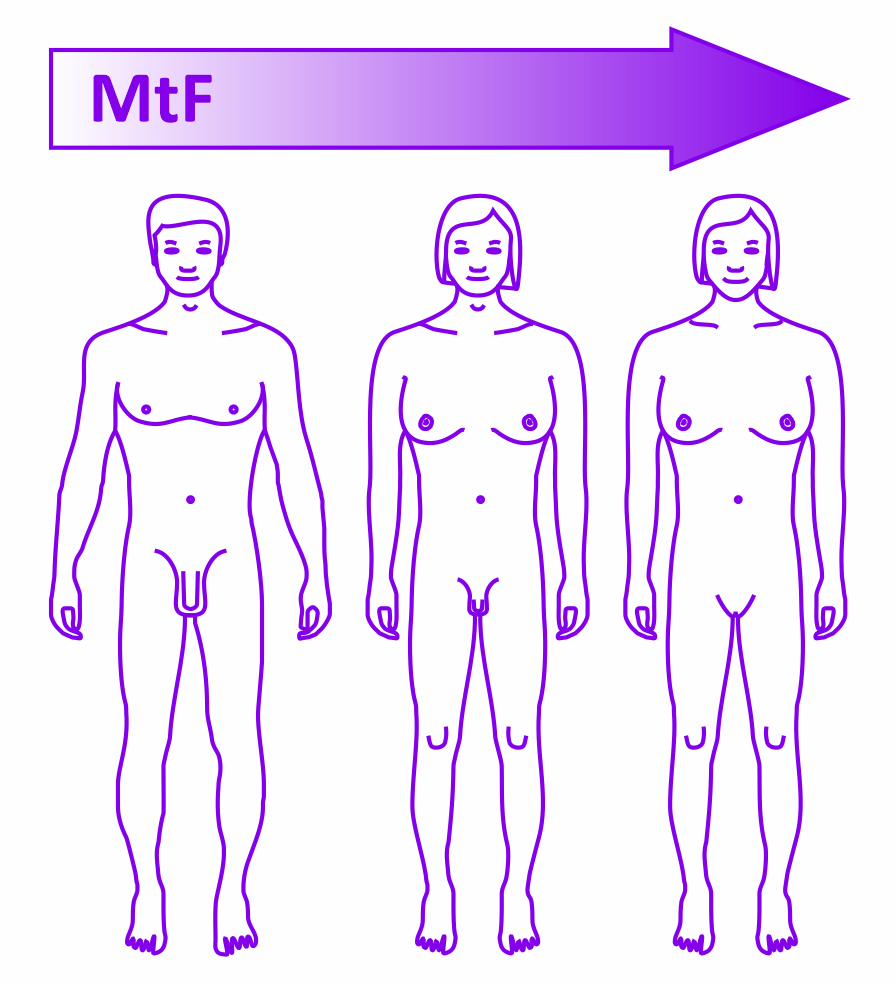
Male to Female
On the transition journey from male to female body characteristics to match a person’s gender identity the effect of oestrogen and antiandrogen can soften the skin and musculature. Body hair can diminish whereas pattern baldness can be reversed. Breast tissue can develop while sperm count decreases and genital size can shrink. Erections can cease and there can be a reduction in sex drive. Voice tone is not affected and may require vocal coaching, along with a need to learn new postural and movement styles. “Top” surgery can be used to soften brow and jawline, remove the Adam’s apple and for breast augmentation. “Bottom” surgery can involve removal of the penis and testes and the creation of a vulva and vagina. It is possible to create a sensate clitoris from part of the glans of the penis. Maintenance of a new vagina requires attentive care.
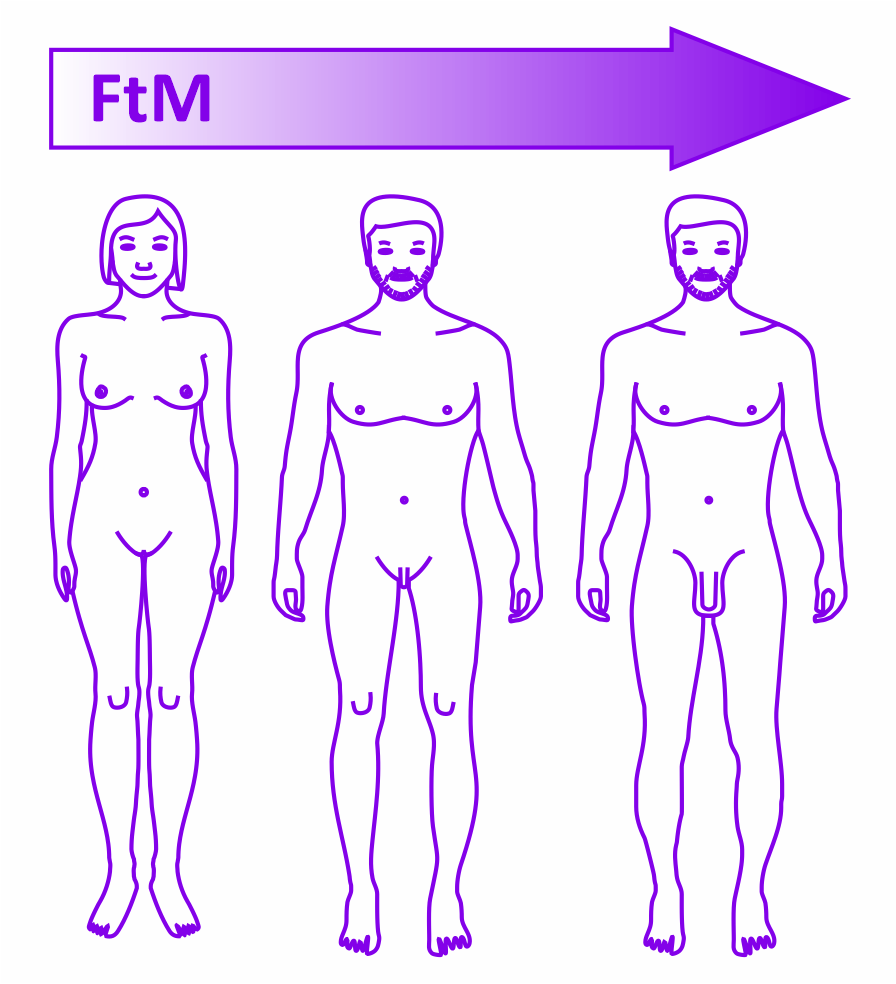
Female to Male
On the transition journey from female to male body characteristics to match a person’s gender identity the effect of testosterone can produce body hair growth and increase muscle mass. There can be an increase in sex drive. Voice tone may shift lower and may benefit from vocal coaching. New postural and movement styles can be learned. Menstruation may cease and the vagina may shrink. The clitoris may grow. “Top” surgery can be used to remove breast tissue and contour the chest. A hysterectomy may be recommended. “Bottom” surgery is invasive and is less common. It may involve re-siting the enlarged clitoris into a more prominent position. It is possible to create a penis and scrotum but they will not have all the characteristics of natural male genitals. For example the remaining clitoris will still be needed for sexual stimulation.
